You know that your body can heal itself in many ways from cut skin to broken bones. But, did you know that there are also many conditions that exceed your body’s ability to repair the damage? In these cases, traditional medicine seeks to relieve symptoms and manage progression, but regenerative medicine takes it a step further and helps the body regenerate and restore itself. That’s right! The answer to stopping your pain is in your own blood! We’re talking about Regenerative Medicine and its most effective and proven innovative treatment called- PRP therapy.
In this blog we’re going to share with you our top 5 rated benefits of this amazing treatment! But first, let’s go over a little more about what Regenerative Medicine is.
What is Regenerative Medicine?
Our bodies have remarkable capacities for self-healing. We see evidence of it every day, from a shaving nick that quickly scabs over to a broken bone that knits itself inside a cast. The body is not only designed to protect itself from disease by way of its immune system, but it’s also designed to repair its own damages using an incredibly sophisticated network of microscopic healing agents. Which is how regenerative medicine became the forefront in revolutionary medicine.
Regenerative Medicine encompasses a wide range of therapies. The core idea behind these regenerative medical techniques is to strategically aim these restoring agents directly toward an injured or compromised area so that worn or damaged tissue can be “rebuilt’ with fresh new tissue. For many painful conditions, regenerative medicine is a revolutionary option that is fast becoming a new standard of care.
One of the most effective and proven innovative treatments under the regenerative medicine umbrella — platelet-rich plasma therapy (PRP) — has been proven particularly effective in orthopedic injuries and diseases.
PRP therapy uses a nutrient-rich concoction of healing agents collected from the patient’s own blood that is injected into the trouble site. From there, these agents not only start to heal and rebuild damaged tissue, but they also summon other bodily healing agents to join them.
At Southcoast Medical in Mt. Pleasant, SC., our team of experienced physicians offers PRP treatments to our patients suffering from sports injuries, arthritis, and other musculoskeletal damage and pain. Here’s what you need to know.
Demystifying PRP
Platelet-rich plasma may sound like a complicated science experiment, but it’s actually quite simple.
We draw a small sample of blood from your arm, just like any normal blood test. Then we process it in a centrifuge, which spins it at a high speed and separates your blood into its different components. We isolate the plasma (the liquid part of your blood), which contains growth factors and proteins essential for blood clotting and healing.
Finally, we inject this concentrated serum into your injured or diseased tissue, where it goes to work stimulating your body’s natural ability to produce reparative cells that regenerate the tissue much faster and more completely than it would on its own.
Our top 5 rated Benefits of PRP therapy
Whether you have a torn ligament, knee osteoarthritis, or plantar fasciitis, your main goal is probably to stop the pain so you can get back to an active life. But masking the pain with drugs is only a temporary fix, and surgery is the last thing you want. PRP addresses the root of the problem, repairing the damage quickly so the pain goes away for good. Here are the advantages of PRP:
1. Reduces healing time
Waiting for your injury to heal is like watching paint dry — the process is long and it’s hard to see progress. PRP is like a fast-forward button for the healing process. It kicks your body’s natural resources into high gear and significantly reduces the time it takes to reach full recovery.
2. Reduces inflammation
When you experience an acute injury, your immune system floods the area with blood to deliver oxygen and other healing properties to the site. But when inflammation sticks around, it hinders healing and worsens pain. That’s why so much emphasis is placed on getting rid of swelling during rehab — elevation, ice, compression, rest, and anti-inflammatory drugs.
But PRP takes care of the problem from the inside out, suppressing inflammatory agents so your tendons, muscles, ligaments, and joints can heal in peace.
3. Minimally invasive
Sometimes surgery is the best and only solution for a particular injury or disease, but let’s face it, we’d all like to avoid going under the knife if at all possible. PRP makes it possible (in many cases).
The only invasion is a needle stick to withdraw a blood sample, and another one to inject the plasma. There’s no downtime involved and no surgical incision to deal with.
4. Low risk
PRP uses your own blood, so there is virtually no risk of an allergic or adverse reaction, and there are no side effects. Although there is a minuscule chance of infection at the injection site, it’s very rare, especially when compared to surgical procedures.
5. Reduces need for medication and surgery
By reducing the amount of time it takes for your tissues to heal, dramatically reducing inflammation and pain, and requiring no incision, PRP can make it possible to avoid drug use completely.
See A PRP Specialist
If you have an acute injury or chronic pain that won’t respond to traditional treatments, schedule a consultation with one of our PRP specialists at Southcoast Medical in Charleston/ Mt. Pleasant, SC
and find out whether the answer to your pain is in your own blood. Book online by Clicking Here or call us today (843) 990-8390
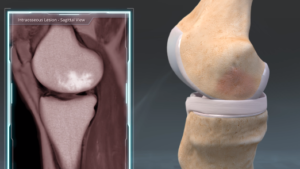 This includes the finding of subchondral edema, a swelling in the bone matrix that may happen from mild fracture, persistent bone bruises, osteoarthritis, and early stages of avascular necrosis. This is quite often the cause of pain in chronic knee arthritis and when treated, can relieve pain.
This includes the finding of subchondral edema, a swelling in the bone matrix that may happen from mild fracture, persistent bone bruises, osteoarthritis, and early stages of avascular necrosis. This is quite often the cause of pain in chronic knee arthritis and when treated, can relieve pain.





