Cell Therapy Efficacy in knee arthritis
Can we reduce pain from Knee Arthritis, and improve mobility, using PRP or BMC?
Knee Arthritis can be very painful and can cause disability, limiting a patient’s lifestyle significantly. According to recent data 40% of people over age 40 have knee arthritis. This causes a substantial strain on our medical system. Traditionally, treatment options are quite limited ending in Total Knee Replacement.  These options include:
These options include:
- Therapy
- Bracing
- NSAIDs
- injectable steroids and hyaluronic acid
- Finally…Total Knee Replacement Surgery
Physicians like me, who have treated patients with joint arthritis for many years, understand the negative consequences of this algorithm. Many patients who have Total Knee Replacement are unhappy. According to materials published by the AARP, as many as1 in 3 patients who undergo total knee replacement are left with chronic pain. Patients know this and are left looking for effective, less invasive options.
One of these options is one of the newer formulations of Hyaluronic acid, like Hymovis, or Durolane. These are typically covered by Medicare, are simple and easy to inject with little or no pain, and can provide fast relief. In our practice, we have been astounded by the number of patients who are unhappy with total knee replacement, had surgery before even trying these simple solutions. We absolutely recommend trying this as a early treatment, if more simple options fail to relieve knee pain. 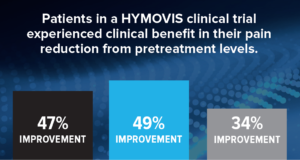
There are some patients who fail to gain improvement from hyaluronic acid or any other of the conservative approaches. Are they destined to go on to Total Knee Replacement?
Maybe not!
Most Orthopedic practices do encourage patients to move forward with Total knee replacement if they continue to have pain. But there are other options for relief, including PRP and the use of Bone Marrow Concentrate (BMC). Though neither of these options is FDA approved, and neither is typically covered by insurance (though sometimes PRP may be), both have a solid scientific basis for use.
This years Orthobiologic Conference (TOBI 2021) included physician presenters from around the world, one of which was Dr. Nicholas Fiz. He reviewed prior data for using PRP to treat knee arthritis, and then presented his own study showing good results in relieving pain and increasing mobility, using PRP. Patients with mild to moderate arthritis had good relief with 3 simple, in office injections of PRP.  Patients with more severe arthritis still did well, but required the injection of PRP into the bone below the damaged cartilage. This included the most severe grade of arthritis with 68% of these patients remaining improved at 15 months post injection.
Patients with more severe arthritis still did well, but required the injection of PRP into the bone below the damaged cartilage. This included the most severe grade of arthritis with 68% of these patients remaining improved at 15 months post injection.
___________________________
With regard to the use of BMC, in 2015 my colleagues published a paper on the use of BMC for the treatment of knee arthritis. You can access the full content here:
This paper, published in the journal of prolotherapy, revealed that:
“The short-term follow up after injection of autologous
BMC and adipose in patients with knee OA showed
excellent results including decreased pain, increased
function, improved activities of daily living and improved
quality of life.”
Though neither PRP nor bone marrow aspirate are approved by the FDA for use to treat arthritis, there are ongoing studies, including a new investigational drug study begun by our group, Bluetail Medical. These studies will take time, and many other studies will be done, but physicians around the world are using these techniques to try to give patients more options and avoid a surgery with less than ideal outcomes like knee replacement.
If you have knee arthritis and limited activity, come see us. Let us guide you through all the Medicare-covered options first. If these don’t work, we would be happy to have a discussion about PRP or BMC.
Contact us anytime:843 990 8390 or Getactiveagain.com







